NJ (908) 688-5577
NY (212) 737-2528

A fungal infection of the toenails can be unsightly. Infected toenails may have white or yellow patches of discoloration, be chalky, or have a crumbly texture. In more severe infections, the toenails may thicken and become deformed and discolored. There are several treatments available for toenail fungus. A podiatrist may prescribe oral antifungal medications, which have to be taken for several months to get full results. Topical treatments, such as medicated nail polishes, are applied directly to the affected nails and can also help treat toenail fungus. Sometimes, both treatments can be used simultaneously. For more information about treatment for toenail fungus, please consult with a podiatrist.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact Glenn Davison, DPM of Advanced Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Symptoms
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
While not a serious issue, toenail fungus, or onychomycosis, can be an embarrassing and uncomfortable condition to experience. Toenail fungus is often caused from public areas that harbor fungi and improper cleaning/drying of the foot. Once infected, the fungus grows deeper into the nail and can be very hard to get rid of.
There are different types of fungus that cause toenail fungus. Dermatophytes, yeasts, and molds are the most frequent forms of fungus to infect the toenail. Dermatophytes are the most common among the three. Symptoms associated with fungal nails include the discoloration of the toenail, brittleness, and in some circumstances, a smell. Pain is rarely a symptom caused by toenail fungus.
Diagnosis of fungal nails is generally a rather quick process. However podiatrists will make sure that the cause is not another condition such as lichen planus, psoriasis, onychogryphosis, or nail damage. Podiatrists will make use of fungal cultures and microscopy to verify that it is fungus.
While over-the-counter ointments are readily available, most are ineffective. This is due to the fact that the nail is very protective and that the fungus slips in between the nail plate and bed. Podiatrists can offer oral medication which currently provides the best results.
Ultimately, prevention is the best line of defense against toenail fungus. Avoid unsanitary public showers. If you do use a public shower, use shower shoes to provide your foot with protection. Once you are finished showering, make sure to thoroughly dry your feet. Fungi thrive in warm, dark, and moist places like sweaty, warm feet that are left dark in shoes all day.
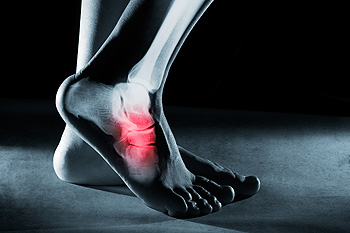 The bone that protrudes on the inside of the ankle is known as the medial malleolus. A stress fracture can occur when this bone and the surrounding area become unbalanced. This may happen as a result of practicing weight-bearing exercises and can gradually cause severe pain and discomfort. Additional reasons why patients may endure a stress fracture can include changing the shoes that are worn during exercising or suddenly increasing exercise intensity levels. Some of the symptoms that can be experienced include a limited range of motion, stiffness, and difficulty walking. There are several treatment options that are available, and it is recommended that you consult with a podiatrist who can determine what the best treatment is for you.
The bone that protrudes on the inside of the ankle is known as the medial malleolus. A stress fracture can occur when this bone and the surrounding area become unbalanced. This may happen as a result of practicing weight-bearing exercises and can gradually cause severe pain and discomfort. Additional reasons why patients may endure a stress fracture can include changing the shoes that are worn during exercising or suddenly increasing exercise intensity levels. Some of the symptoms that can be experienced include a limited range of motion, stiffness, and difficulty walking. There are several treatment options that are available, and it is recommended that you consult with a podiatrist who can determine what the best treatment is for you.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Glenn Davison, DPM from Advanced Podiatry. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
Certain medical conditions, such as peripheral artery disease, can cause poor circulation in the legs, feet, and ankles. Vascular tests are used by podiatrists to examine the blood flow in the lower limbs. While this may sound potentially painful, most vascular tests used by podiatrists are actually noninvasive and fairly painless. Examples of vascular tests that a podiatrist might use include the ankle-brachial index, which measures the blood pressure at your ankle and at your arm and then compares the two readings, or the Doppler ultrasound, which uses sound waves to visualize your blood flow on a computer screen. For more information about vascular tests in podiatry, consult with a podiatrist today.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with Glenn Davison, DPM from Advanced Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
In foot care, vascular testing may be required in the diagnosing and treatment of certain podiatric conditions. Vascular testing is particularly relevant for patients with high-risk diabetes, poor circulation, peripheral artery disease (PAD), and chronic venous insufficiency (CVI). Procedures typically involve the examination of blood vessels throughout the body for blockages or buildup.
Vascular testing is very important for the diagnosis of various conditions, including peripheral artery disease and chronic venous insufficiency, as these conditions can greatly affect one’s quality of life and cause pain in the lower limbs. Circulatory problems in the feet and ankles can reflect issues throughout the body, making testing of the blood vessels pertinent.
Testing methods vary between practitioners and can be specific to certain foot and ankle problems. Modern technology has brought about the ability to perform vascular testing using non-invasive methods, such as the cuff-based PADnet testing device. This device records the Ankle-Brachial Index (ABI)/Toe-Brachial Index (TBI) values and Pulse Volume Recording (PVR) waveforms. Contact your podiatrist to determine what vascular testing is available for your needs.
 There is a condition that can affect the feet and cause them to sweat excessively. This is referred to as plantar hyperhidrosis. Generally, one of the most common side effects is that the excessive sweat causes discomfort due to the sogginess of the socks and shoes. People afflicted with this condition tend to go through shoes quicker because of the salt mineral within the sweat. Plantar hyperhidrosis can also lead to embarrassment and avoidance of activities. Fortunately, treatments for this condition are available. If you are experiencing excessively sweaty feet, it is suggested that you consult with a podiatrist. A podiatrist can diagnose your condition and find the correct treatment for you.
There is a condition that can affect the feet and cause them to sweat excessively. This is referred to as plantar hyperhidrosis. Generally, one of the most common side effects is that the excessive sweat causes discomfort due to the sogginess of the socks and shoes. People afflicted with this condition tend to go through shoes quicker because of the salt mineral within the sweat. Plantar hyperhidrosis can also lead to embarrassment and avoidance of activities. Fortunately, treatments for this condition are available. If you are experiencing excessively sweaty feet, it is suggested that you consult with a podiatrist. A podiatrist can diagnose your condition and find the correct treatment for you.
If you are suffering from hyperhidrosis contact Glenn Davison, DPM of Advanced Podiatry. Our doctor can provide the care you need to attend to all of your foot and ankle needs.
Hyperhidrosis of the Feet
Hyperhidrosis is a rare disorder that can cause people to have excessive sweating of their feet. This can usually occur all on its own without rigorous activity involved. People who suffer from hyperhidrosis may also experience sweaty palms.
Although it is said that sweating is a healthy process meant to cool down the body temperature and to maintain a proper internal temperature, hyperhidrosis may prove to be a huge hindrance on a person’s everyday life.
Plantar hyperhidrosis is considered to be the main form of hyperhidrosis. Secondary hyperhidrosis can refer to sweating that occurs in areas other than the feet or hands and armpits. Often this may be a sign of it being related to another medical condition such as menopause, hyperthyroidism and even Parkinson’s disease.
In order to alleviate this condition, it is important to see your doctor so that they may prescribe the necessary medications so that you can begin to live a normal life again. If this is left untreated, it is said that it will persist throughout an individual’s life.
A last resort approach would be surgery, but it is best to speak with your doctor to find out what may be the best treatment for you.
If you have any questions please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Hyperhidrosis of the feet, also termed plantar hyperhidrosis, is characterized by excessive sweating of the feet that can be onset by any cause, such as exercise, fever, or anxiety. Most people suffering from hyperhidrosis of the feet also experience hyperhidrosis of the hands, or palmar hyperhidrosis. Approximately 1-2% of Americans suffer from this disorder.
Sweating is a healthy process utilized by the body in order to cool itself and maintain a proper internal temperature, which is controlled by the sympathetic nervous system. In individuals with hyperhidrosis, the sympathetic nervous system works in "overdrive", producing far more sweat than is actually needed.
Plantar hyperhidrosis is considered primary hyperhidrosis. Secondary hyperhidrosis refers to excessive sweating that occurs in an area other than the feet, hands, or armpits, and this indicates that is related to another medical condition, such as menopause, hyperthyroidism, or Parkinson's disease.
Symptoms of hyperhidrosis of the feet can include foot odor, athlete's foot, infections, and blisters. Because of the continual moisture, shoes and socks can rot which creates an additional foul odor and can ruin the material, requiring shoes and socks to be replaced frequently. In addition to the physical symptoms, emotional health is often affected as this disorder can be very embarrassing.
If left untreated, hyperhidrosis will usually persist throughout an individual's life. However, there are several treatment options available. A common first approach to treating hyperhidrosis of the feet is a topical ointment. Aluminum chloride, an ingredient found in antiperspirants, can be effective at treating hyperhidrosis if used in high concentration and applied to the foot daily. Some individuals can experience relief this way, while others encounter extreme irritation and are unable to use the product. Another procedure is the use of Botulinum Toxin A, commonly referred to as Botox. This is injected directly into the foot, and is effective at minimizing the sweat glands in the injected area. These injections must be repeated every 4 to 9 months.
If these treatments are ineffective, oral prescription medications may be taken in an effort to alleviate the symptoms. Again, some will experience relief while others do not. Going barefoot reportedly provides relief for most sufferers.
A final approach to combating hyperhidrosis of the feet is through surgery. Surgery has been less successful on patients with plantar hyperhidrosis than on those with palmar hyperhidrosis. It is only recommended when sweating is severe and other treatments have failed to work. This kind of surgery usually involves going into the central nervous system, and cutting nerves to stop the transmission of signals telling the foot to sweat.
 One of the functions of the cuboid bones is to maintain stability and mobility while walking. The pain that can result from a cuboid bone injury is generally felt on the outside of the foot, and causes difficulty walking and running. Cuboid syndrome can happen suddenly, and patients may develop this condition from incurring an ankle sprain. Additionally, it may occur from frequently wearing high heels or in athletes who participate in jumping activities. Mild relief may be found when weight is taken off of the affected foot, which can make it easier to move the foot. After a proper diagnosis is given, there may be specific stretches that can be practiced which can promote healing. If you have pain in this part of your foot, it is suggested that you confer with a podiatrist who can effectively treat this condition.
One of the functions of the cuboid bones is to maintain stability and mobility while walking. The pain that can result from a cuboid bone injury is generally felt on the outside of the foot, and causes difficulty walking and running. Cuboid syndrome can happen suddenly, and patients may develop this condition from incurring an ankle sprain. Additionally, it may occur from frequently wearing high heels or in athletes who participate in jumping activities. Mild relief may be found when weight is taken off of the affected foot, which can make it easier to move the foot. After a proper diagnosis is given, there may be specific stretches that can be practiced which can promote healing. If you have pain in this part of your foot, it is suggested that you confer with a podiatrist who can effectively treat this condition.
Cuboid syndrome, also known as cuboid subluxation, occurs when the joints and ligaments near the cuboid bone in the foot become torn. If you have cuboid syndrome, consult with Glenn Davison, DPM from Advanced Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Cuboid syndrome is a common cause of lateral foot pain, which is pain on the outside of the foot. The condition may happen suddenly due to an ankle sprain, or it may develop slowly overtime from repetitive tension through the bone and surrounding structures.
Causes
The most common causes of cuboid syndrome include:
Symptoms
A common symptom of cuboid syndrome is pain along the outside of the foot which can be felt in the ankle and toes. This pain may create walking difficulties and may cause those with the condition to walk with a limp.
Diagnosis
Diagnosis of cuboid syndrome is often difficult, and it is often misdiagnosed. X-rays, MRIs and CT scans often fail to properly show the cuboid subluxation. Although there isn’t a specific test used to diagnose cuboid syndrome, your podiatrist will usually check if pain is felt while pressing firmly on the cuboid bone of your foot.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are ice therapy, rest, exercise, taping, and orthotics.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.