NJ (908) 688-5577
NY (212) 737-2528

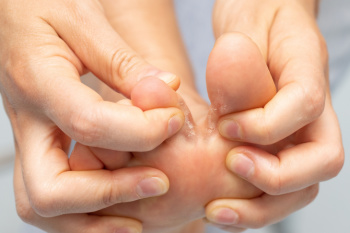 Athlete's foot, also known as tinea pedis, is a fungal infection that primarily affects the spaces between the toes. Anyone exposed to the fungus can become infected, not just athletes. Dermatophytes, the fungi responsible for this condition, thrive in warm, moist environments, making hot, sweaty feet the perfect breeding ground. Symptoms can include redness, cracking, flaking, and itching of the skin, particularly between the toes. Athlete's foot is extremely contagious, spreading through direct contact or via contaminated surfaces like gym locker rooms and communal showers at indoor pools. Risk factors can include eczema, excessive sweating, weakened immune systems, circulation problems, and wearing sturdy, non-breathable footwear. A podiatrist can diagnose athlete’s foot and recommend effective treatments as well as provide preventive measures to keep the infection from recurring. If you have developed an athlete's foot infection, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
Athlete's foot, also known as tinea pedis, is a fungal infection that primarily affects the spaces between the toes. Anyone exposed to the fungus can become infected, not just athletes. Dermatophytes, the fungi responsible for this condition, thrive in warm, moist environments, making hot, sweaty feet the perfect breeding ground. Symptoms can include redness, cracking, flaking, and itching of the skin, particularly between the toes. Athlete's foot is extremely contagious, spreading through direct contact or via contaminated surfaces like gym locker rooms and communal showers at indoor pools. Risk factors can include eczema, excessive sweating, weakened immune systems, circulation problems, and wearing sturdy, non-breathable footwear. A podiatrist can diagnose athlete’s foot and recommend effective treatments as well as provide preventive measures to keep the infection from recurring. If you have developed an athlete's foot infection, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact Glenn Davison, DPM from Advanced Podiatry. Our doctor will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Athlete’s foot, or tinea pedis, is a skin disease caused by a fungal infection. The infection typically occurs between the toes, and the feet are most subject to this disease because shoes best create the warm, dark, and moist environment in which fungus thrives. Other areas that create a similar environment, such as swimming pools, public showers, and locker rooms; can also promote fungi growth.
Symptoms of athlete’s foot include dry skin, itching, scaling, inflammation, and blistering. Sometimes, blisters can evolve into the cracks or breaks in the skin. The exposed tissue can then create pain, swelling, and discharge. The spread of infection can cause itching and burning as well.
While athlete’s foot commonly occurs between the toes, it may also spread to the toenails or soles of the feet. Other parts of the body, such as the groin or underarms, can also become infected if they are touched after the original area of infection is scratched. Aside from physical contact, athlete’s foot can also spread through the contamination of footwear, clothing or bedsheets.
Proper foot hygiene is essential in preventing athlete’s foot. You can prevent the fungus from spreading by frequently washing your feet using soap and water, thoroughly drying the feet between the toes, changing shoes and socks every day to reduce moisture, and ensuring that bathroom and shower floors are disinfected. Other tips include using shower shoes, avoiding walking barefoot in public environments, wearing light and airy shoes, and wearing socks that keep the feet dry.
While treatment for athlete’s foot can involve topical or oral antifungal drugs, mild cases of the infection can be treated by dusting foot powder in shoes and socks. Any treatment used can be supplemented by frequently bathing the feet and drying the toes. If proper foot hygiene and self-care do not ease your case of athlete’s foot, contact your podiatrist. He will determine if the underlying cause of your condition is truly a fungus. If that is the case, a comprehensive treatment plan may be suggested with the inclusion of prescription antifungal medications.
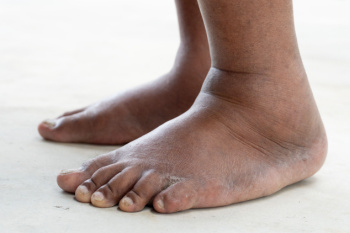 Swelling of the feet, also known as edema, is a condition that results from an abnormal accumulation of fluid in the tissues of the feet and ankles. This swelling can be caused by various factors, including standing or sitting for long periods, pregnancy, or obesity. Injury, or underlying health conditions like heart disease or kidney problems are other risk factors. Swollen feet can be uncomfortable, may restrict mobility, and can make daily tasks difficult to complete. Often, simple changes in regimen, such as elevating the feet, wearing compression socks, staying hydrated, and engaging in regular exercise may reduce the amount of swelling in the feet. If swelling persists or is accompanied by other concerning symptoms, it is suggested to seek evaluation and treatment from a podiatrist to ensure proper management and prevent complications.
Swelling of the feet, also known as edema, is a condition that results from an abnormal accumulation of fluid in the tissues of the feet and ankles. This swelling can be caused by various factors, including standing or sitting for long periods, pregnancy, or obesity. Injury, or underlying health conditions like heart disease or kidney problems are other risk factors. Swollen feet can be uncomfortable, may restrict mobility, and can make daily tasks difficult to complete. Often, simple changes in regimen, such as elevating the feet, wearing compression socks, staying hydrated, and engaging in regular exercise may reduce the amount of swelling in the feet. If swelling persists or is accompanied by other concerning symptoms, it is suggested to seek evaluation and treatment from a podiatrist to ensure proper management and prevent complications.
Swollen feet can be a sign of an underlying condition. If you have any concerns, contact Glenn Davison, DPM of Advanced Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Swollen feet are a common ailment among pregnant women and people who stand or sit for extended periods. Aging may increase the possibility of swollen feet and patients who are obese often notice when their feet are swelling too. There may be medical reasons why swollen feet occur:
Swollen feet can also be caused by bone and tendon conditions, including fractures, arthritis, and tendinitis. Additionally, there may be skin and toenail conditions and an infection may cause the feet to swell. Patients who take medicine to treat high blood pressure may be prone to getting swollen feet.
Many patients elevate their feet to help relieve the swelling and this is generally a temporary remedy. When a podiatrist is consulted the reason behind the swelling can be uncovered and subsequently treated.
If you have any questions please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
There are many reasons why patients experience swelling of the feet. It is rather common and may be a side effect of pregnancy or from sitting and standing for most of the day. Gravity could also play a role in the development of swollen feet. It is known that the weight of blood volume in our bodies is exerted on the veins in the legs and feet. The veins may not work as efficiently during the aging process, and this could make the blood flow backward causing swollen feet. Relief may be found when obese patients lose weight, and it may help to engage in compression therapy by wearing compression socks, stockings, or athletic sleeves. This method can release pressure on the feet and ankles which may help to reduce existing swelling. There are patients who have controlled their swollen feet by implementing healthy lifestyle changes. These can consist of reducing salt intake, incorporating a gentle exercise regime into the daily routine, and drinking plenty of fresh water. Swollen feet may be a temporary condition that affects people who travel via airplane or automobile, so it is beneficial to walk as frequently as possible even though it can be difficult. Swelling of the feet can also be indicative of other health issues so it is important to pay attention to any type of chest pain, mental confusion, dizziness, or fever. If you consistently have swollen feet, it is strongly suggested that you consult with a podiatrist who can help determine the cause and how to effectively treat it.
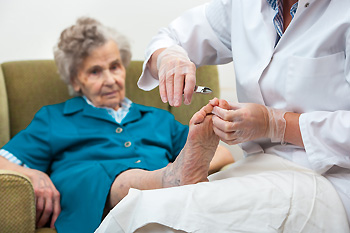 Foot exams are important for older adults, as aging often brings about various foot problems that can significantly impact mobility and increase the risk of falls. Over time, feet undergo changes such as loss of fat padding, reduced blood circulation, and structural alterations, making them more susceptible to conditions like arthritis, bunions, and plantar fasciitis. Additionally, common age-related issues like diabetes can lead to neuropathy and other complications that exacerbate foot problems. Regular foot care becomes more critical with age, as maintaining foot health directly contributes to overall well-being and independence. If self-care becomes challenging, it is essential to seek assistance from caregivers or healthcare professionals to ensure proper hygiene and monitoring. Routine foot exams involve checking for signs of skin breakdown, infections, deformities, and circulation issues. A podiatrist may also assess gait and balance to prevent falls. If you are a senior, it is suggested that you schedule an appointment with a podiatrist for comprehensive foot care, as they specialize in diagnosing and treating foot-related issues.
Foot exams are important for older adults, as aging often brings about various foot problems that can significantly impact mobility and increase the risk of falls. Over time, feet undergo changes such as loss of fat padding, reduced blood circulation, and structural alterations, making them more susceptible to conditions like arthritis, bunions, and plantar fasciitis. Additionally, common age-related issues like diabetes can lead to neuropathy and other complications that exacerbate foot problems. Regular foot care becomes more critical with age, as maintaining foot health directly contributes to overall well-being and independence. If self-care becomes challenging, it is essential to seek assistance from caregivers or healthcare professionals to ensure proper hygiene and monitoring. Routine foot exams involve checking for signs of skin breakdown, infections, deformities, and circulation issues. A podiatrist may also assess gait and balance to prevent falls. If you are a senior, it is suggested that you schedule an appointment with a podiatrist for comprehensive foot care, as they specialize in diagnosing and treating foot-related issues.
If you need your feet checked, contact Glenn Davison, DPM of Advanced Podiatry. Our doctor will attend to all of your foot and ankle needs and provide you with quality treatment.
Geriatrics and Podiatry
When people age, some common issues that may occur are bone density loss, dry skin, poor circulation, and rough brittle nails. These issues may also affect your foot health if the necessary steps are not taken to alleviate the problems.
It is important to take care of your feet because feet that are injured or diseased can affect your overall health. Having painful feet hinders your ability to do daily activities or may decrease your willingness to do the things that you need to do.
Visiting Your Geriatrician
As we age, health problems become more likely, so it is essential to visit your doctor for check-ups to ensure that you are doing the best you can to take care of your health. It is recommended to check your feet frequently for any possible cuts, bruises, swelling, corns or any other irregularities.
Taking Care of Elderly Feet
Cracked or dry feet can be treated by applying moisturizer often. It is also important not to wear old socks because the older the sock is, the higher the possibility there will be that there is bacteria there. Wear fresh socks and make sure they fit properly.
Proper foot health means that you can have a more active lifestyle and you will not be bogged down by pain. Foot health also leads to good circulation, which is paramount for overall health.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Bone density loss, dry skin, poor circulation, and rough and brittle nails are some of the common problems that can occur as people age. The effect that these problems has on foot health should be of particular concern in comprehensive geriatric care.
Feet that are diseased or injured have a negative effect on overall health and safety. Painful feet limit a person’s willingness and ability to stay active. Poor foot health can also cause gait change, which can lead to falls and accidents. Even though recovery time from health problems naturally slows as we age, many foot problems can be avoided altogether with regular prophylactic care.
Feet should be thoroughly washed in warm water daily. Care must be taken to dry the feet well, making sure to dry between and under the toes. Any left-over moisture can cause problems like foot fungus. After cleaning feet carefully check for problems such as cracked skin, bruises, swelling, cuts, corns, or other irregularities.
Examine toenails for ingrown, jagged, or split nails. Long toenails should be cut straight across. Never cut toenails at an angle or down the side as this may lead to ingrown nails.
Cracked and dry feet should be treated once or twice a day with a non-greasy moisturizer. Rub the moisturizer into the skin and allow it to dry before putting on socks and shoes. Sweaty feet can be dusted with a small amount of talcum powder. Avoid putting talcum directly into shoes as this may make feet slip within the shoe and cause a serious fall.
Wear clean dry socks each day. Not only do clean socks feel better on the feet, but socks worn for longer periods may harbor disease and odor-causing bacteria. Socks should not be tight around the top as they can leave marks on the leg. Socks that are too small can bring about bruising caused by pressure against the toes.
Wear comfortable and well-fitting shoes. If possible, consult a professional footwear specialist when purchasing shoes. Do not walk around barefoot as this exposes the feet to possible injury and bacteria.
Good foot health allows a more active lifestyle, which improves blood flow. Good circulation aids in recovery from injury or illness. It is also important for maintaining overall health.
Serious health problems can manifest themselves as symptoms in the feet. The elderly should seek professional help from a podiatrist if experiencing foot problems like tingling, numbness, pain, infection, or a sore that does not heal. Taking care of these problems right away can prevent the development of severe cases.

Foot blisters are small, fluid-filled pockets that form on the upper layers of the skin, typically caused by friction. These blisters often develop due to repetitive rubbing against shoes or socks during activities such as walking, running, or hiking. When the skin experiences constant friction, the outer layer separates from the underlying layers, creating a space that fills with fluid. Moisture from sweat can exacerbate this process, making blisters more likely. Common areas for foot blisters include the heels, toes, and soles. While generally not serious, blisters can be painful and impact mobility. To prevent blisters, it is important to wear well-fitting shoes and moisture-wicking socks, and to keep feet dry. If a blister forms, it should be kept clean and protected to prevent infection and promote healing, and avoiding further irritation is vital for recovery. Foot blisters are often uncomfortable, and can hinder completing daily tasks. If you have a blister on your foot that has become infected, it is suggested that you visit a podiatrist who can offer relief and treatment techniques.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact Glenn Davison, DPM of Advanced Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blisters are pockets of fluid that occur under the top layer of your skin. These fluid pockets are usually filled with pus, blood, or serum. Blisters may itch or hurt and can appear as a single bubble or in clusters.
The most common types of blisters are friction blisters. This type of blister may be caused by wearing shoes that are too tight. Friction blisters can also occur on the hands. A change in temperature may also cause blisters on the feet. In the freezing air, frostbite on your toes can lead to blisters, as well as sunburn from hot weather.
The best way to treat a blister is to keep it clean and dry. Most blisters will get better on their own. Once the skin absorbs the fluid within the blister, it will flatten and eventually peel off. You should avoid popping your blister unless you podiatrist does it for you. Additional treatment options include applying an ice pack to the blister or using over-the-counter blister bandages to cover the affected area.
If your blister becomes discolored, inflamed, or worsens it is advised that you speak to your podiatrist. Blisters that are yellow, green, or purple may be infected and require immediate medical attention. Blisters that are abnormally colored may be a sign of a more serious underlying health condition such as herpes.
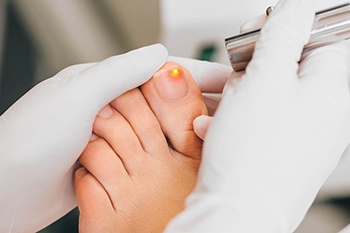
Laser treatment for toenail fungus is an advanced method that uses focused light beams to target and eliminate fungal infections beneath the toenail. This non-invasive procedure penetrates the nail without damaging surrounding tissues, making it a preferred option for many patients. Unlike traditional treatments, such as topical creams or oral medications, laser therapy has minimal side effects and a higher success rate. The procedure is typically quick, often completed in under an hour, and requires no downtime, allowing patients to resume normal activities immediately. Multiple sessions may be needed for optimal results, depending on the severity of the infection. Laser treatment is effective for many individuals, offering a promising solution for persistent toenail fungus, especially for those who have not responded well to other treatments. Toenail fungus can be unsightly, and is treated by a podiatrist. If you have this condition, it is suggested that you consult this type of doctor who can determine if laser therapy is right for you.
Laser treatment can be an effective way to get rid of toenail fungus. If you have any questions about laser treatment, consult with Glenn Davison, DPM from Advanced Podiatry. Our doctor will assess your condition and provide you with quality treatment for fungal nails.
What Are Toenail Fungal Infections?
Onychomycosis, or fungal infection of the nail, is a relatively common and non-serious condition. Around 10 percent of U.S. citizens are afflicted with fungal nails. Common forms of fungus that infect the nail include dermatophytes, yeasts, and molds.
Symptoms of Toenail Fungal Infections Include:
Diagnosis for Fungal Nails
Fungal infections are diagnosed by fungal culture and microscopy. This will rule out any other conditions such as nail trauma, psoriasis, lichen planus, and onychogryphosis.
What Is Laser Treatment?
Laser treatment is a non-invasive, safe, quick, and painless procedure that uses the heat from a laser to kill fungus in the nail. Each infected nail is targeted with a laser for several minutes. The treatment is usually utilized several different times over a select period. During this time, a podiatrist will keep an eye on the infection.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.